Milia: What They Are, Why They Appear & Safe Doctor-Led Removal with Advanced Electrocautery in Hale, Cheshire
Milia are one of the most common (and most misunderstood) reasons patients book to see me for “white bumps” on the face particularly around the eyes. They’re often mistaken for whiteheads, yet no amount of exfoliating, acids, squeezing, or retinoids seems to shift them. In fact, DIY attempts can make things worse.
In this guide, I’ll explain what milia really are, why they form, and how we remove them safely using precise medical electrocautery/electrosurgery at our doctor-led clinic in Hale, serving patients from Altrincham and South Manchester.
What Are Milia?
A milium (singular) is a tiny cyst filled with keratin (a natural skin protein). When there are several, we call them milia. They sit just under the skin surface and look like small pearly-white or yellowish bumps. (DermNet®)
Typical features:
1–2 mm, firm, dome-shaped
Usually not red or inflamed
Commonly on the eyelids and cheeks, but can also appear on the forehead, jawline, and occasionally the body (DermNet®)
Why they can’t be “popped”
Unlike spots, milia usually don’t have an open pore to the surface, so squeezing rarely works and often causes trauma.
Why Do Milia Form?
Milia develop when keratin becomes trapped instead of shedding normally. Contributing factors can include:
Skin barrier disruption (irritation, eczema-prone skin)
Occlusive/heavy products (especially around the eyes)
Sun damage and ageing, which can slow natural shedding
Topical steroid use, including facial/eyelid preparations in some cases
Secondary milia after skin trauma (e.g., procedures, burns, rashes, healing skin) (Primary Care Dermatology Society)
Some people are simply more prone to milia and can form them repeatedly even with excellent skincare.
Why Skincare Alone Usually Doesn’t Remove Established Milia
Skincare can be helpful for prevention, but established milia can be stubborn because they sit beneath intact skin.
Exfoliating acids often don’t penetrate to the cyst
Retinoids may reduce new milia formation in some people, but they rarely “erase” existing ones quickly
Over-exfoliation can irritate the barrier, which may trigger more bumps (DermNet®)
When to Get a Doctor to Check “White Bumps”
Most milia are harmless. However, not every white bump is a milium. Around the eyes in particular, lookalikes can include syringomas, xanthelasma, sebaceous hyperplasia, and other benign lesions—each with different management. (NCBI)
Book an assessment if a lesion:
changes, grows quickly, bleeds, crusts, or becomes painful
is very close to the lash line
keeps recurring in the same spot
Safe Milia Removal: What Actually Works
For individual milia, the most effective approach is usually controlled de-roofing/opening and evacuation performed by a trained clinician using sterile technique. (NCBI)
For multiple milia, or where we want extra precision (especially near the eyes), electrocautery/electrodesiccation can be an excellent option. (DermNet®)
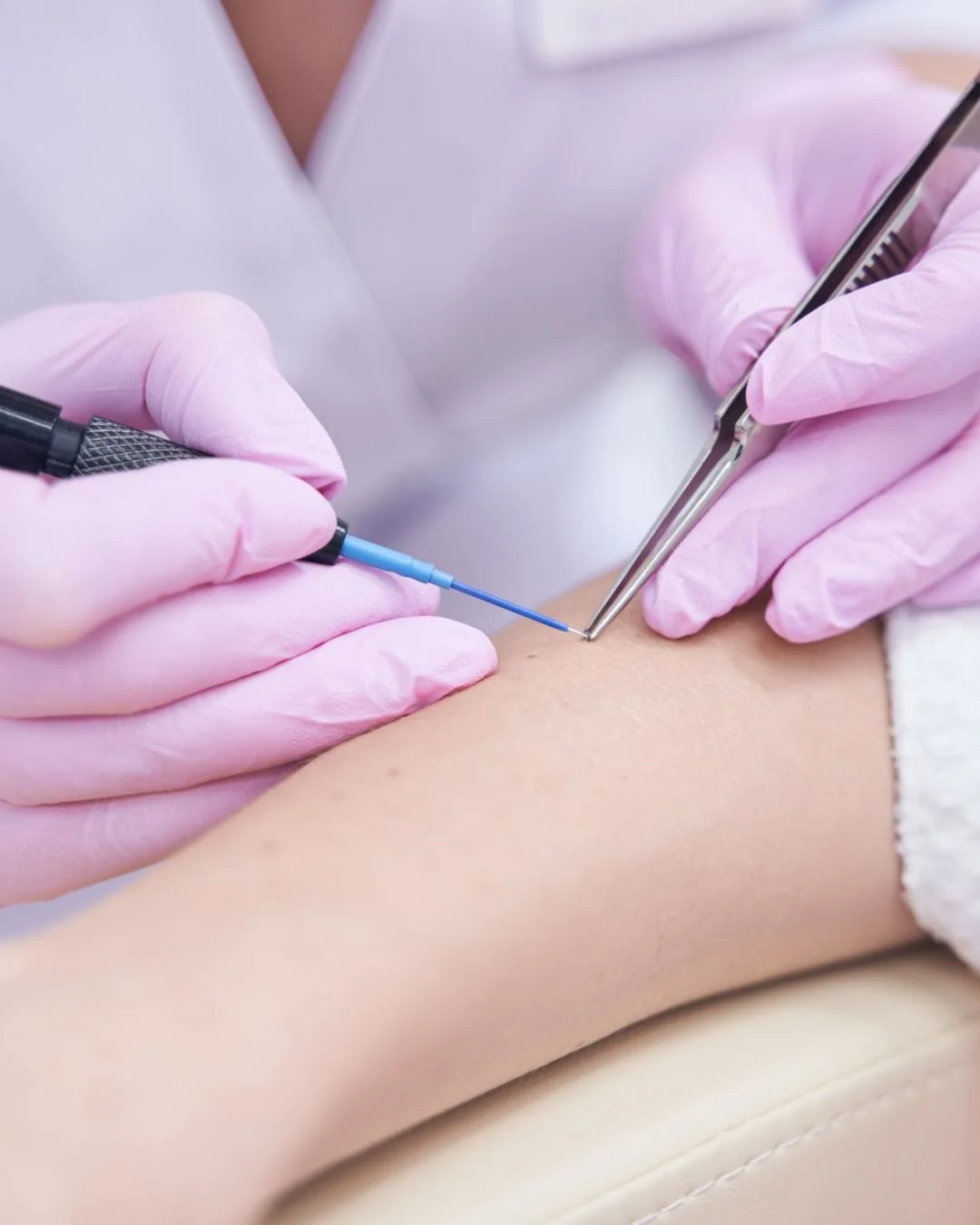
How Advanced Electrocautery Treats Milia (Doctor-led technique)
In clinic, electrocautery/electrosurgery uses a very fine tip and carefully selected settings to:
create a micro-opening (or gently desiccate the lesion)
allow the keratin cyst to be released/removed
produce a very small dry coagulum on the surface which protects the area while it heals (DermNet®)
Why patients like this approach:
precise and efficient for clusters
minimal surrounding skin trauma when performed correctly
particularly useful for delicate areas such as peri-orbital skin (DermNet®)
Why Doctor-Led Treatment Matters (Especially Around the Eyes)
The eyelid area is unforgiving: the skin is thin, vascular, and close to important structures. A doctor-led approach matters because we:
confirm the diagnosis (not all “milia” are milia)
choose the safest technique and depth
reduce avoidable risks such as infection, pigment change, scarring, or prolonged redness
tailor aftercare to sensitive skin types (eczema/rosacea-prone) (NCBI)
What We Can Treat in One Appointment
Depending on the number, location, and your skin sensitivity, we can often treat multiple benign concerns in one visit, for example:
Milia + skin tags
Milia + cherry angiomas (“blood spots”)
Milia + thread veins (if suitable)
Everything is assessed and planned individually.
Pricing & Appointment Details (Hale, Cheshire)
30-minute appointment: £220
Includes:
Doctor-led consultation and skin assessment
Treatment time (often ~15 minutes of active treatment within the appointment)
In many sessions we can treat multiple concerns (e.g., milia + skin tags / blood spots), depending on complexity and comfort.
Add extra treatment time: +15 minutes for £99
Ideal if you have numerous milia or multiple areas.
Typical averages treated in ~15 minutes (estimates)
Milia: ~10
Skin tags: ~5 (depending on type/size)
Thread veins: ~2–3 cm of vessels
Cherry angiomas/blood spots: ~5–8
Follow-up (if needed)
Most milia improve immediately and settle with one session. If further treatment is required:
£150
Usually spaced 4+ weeks apart
This is uncommon but may be needed for extensive or recurrent cases.
Consultation-only option
£50
If you proceed with treatment later, the £50 is deducted from your treatment cost
A consultation-only appointment may be advised if diagnosis is uncertain, the lesion is extremely close to the eye margin, or you have a complex medical/skin history.
Patch Test Option (For Sensitive or Reactive Skin)
A patch test may be recommended if you:
have very reactive skin or eczema
have a history of pigment change after inflammation
tend to heal slowly
want extra reassurance before treating visible facial areas
We treat a small discreet area first, then review healing at 3–4 weeks before proceeding.
Healing & Aftercare: What to Expect
After milia removal, it’s normal to have:
mild redness
tiny surface scabs/crusts
healing typically over 5–10 days (varies by area and skin type)
Aftercare is simple but important:
gentle cleansing
avoid picking or exfoliating
pause strong actives (retinoids/acids) until healed
daily SPF to reduce post-inflammatory pigment risk
Most patients return to normal routine immediately (with a few skincare tweaks).
Milia Removal in Hale, Altrincham & South Manchester
If you’re looking for safe, effective milia removal in Hale, in a calm medical environment—with patients regularly travelling from Altrincham and across South Manchester—this is exactly the kind of “small procedure, big confidence boost” we do every week.
We’re a female-led, family-run, doctor-led clinic focused on:
careful diagnosis and skin-first decisions
precise, conservative treatment
excellent aftercare and long-term skin health
Frequently Asked Questions (FAQ)
Are milia acne?
No. Milia are keratin cysts, not acne lesions or “dirty pores.” (DermNet®)
Can milia go away on their own?
They can—particularly in babies. In adults they often persist, especially around the eyes. (DermNet®)
Can I remove milia myself?
I wouldn’t recommend it, especially near the eyes. DIY removal increases risk of infection, broken capillaries and scarring. (NCBI)
Does retinol or tretinoin remove milia?
Retinoids can help reduce new milia in some people, but established milia often require physical removal. (NCBI)
Is electrocautery safe around the eyes?
When performed by an experienced medical clinician with correct settings and technique, it can be a safe, precise option for peri-orbital lesions. (DermNet®)
Will it scar?
Scarring is uncommon when milia are treated correctly and aftercare is followed—but no skin procedure is zero-risk. Your individual risk depends on location, skin type, and healing history.
How painful is it?
Most patients describe brief, sharp discomfort rather than ongoing pain. The procedure is quick.
How long will it take to heal?
Most areas settle over 5–10 days, with tiny scabs that fall away naturally.
Can I wear makeup afterwards?
Often yes (depending on location), but we’ll advise you based on the treated area—many patients prefer to avoid makeup for 24 hours if possible.
Can milia come back?
A treated milium usually doesn’t return, but new milia can form over time—especially if your skin is prone or you use heavy/occlusive products. (DermNet®)
What if it isn’t milia?
That’s exactly why assessment matters. Several benign lesions mimic milia and need different management. (Primary Care Dermatology Society)
Scientific References
DermNet NZ. Milium, milia (clinical features, causes, treatment options). (DermNet®)
Avila PPG, et al. Milia (StatPearls, NCBI Bookshelf) (overview + treatment options including electrocautery/electrodesiccation). (NCBI)
DermNet NZ. Electrosurgery (electrodesiccation indications including milia; mechanism and healing). (DermNet®)
Primary Care Dermatology Society (PCDS). Milia (UK clinical guidance and management overview). (Primary Care Dermatology Society)
Patient.info. Milia: Causes & Treatment (patient-friendly overview written by clinicians). (Patient)
Thami GP, Kaur S, Kanwar AJ. Enucleation of milia with a disposable hypodermic needle (JAAD surgical pearl). (jaad.org)
Janeczek M. Forceps for Milia Extraction (Cutis, 2022; discusses techniques including electrocautery/electrodesiccation). (cdn.mdedge.com)