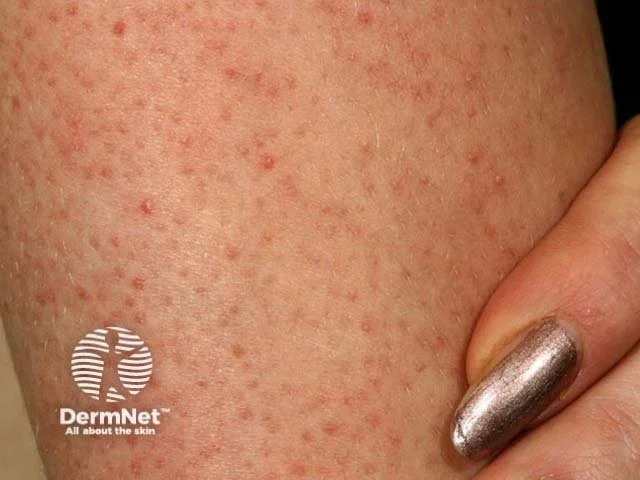
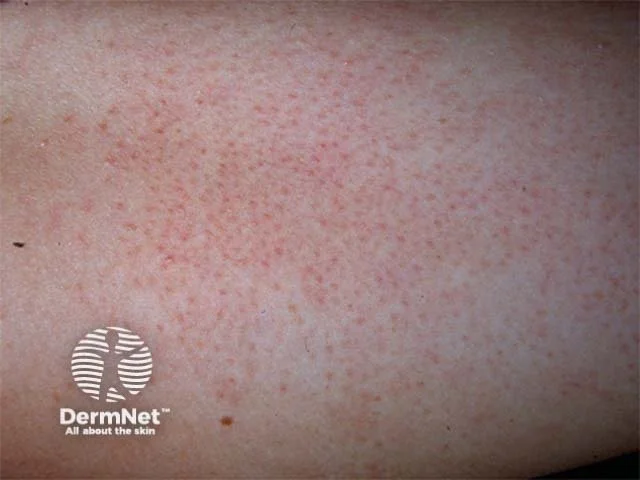
Keratosis Pilaris: The “Chicken Skin” Condition That Isn’t Just Dry Skin
Keratosis pilaris (KP) is often dismissed as a minor cosmetic issue “just dry skin” or “blocked pores.” In reality, it’s a genetic condition of keratinisation that behaves very differently from acne or simple dryness. For many people, it’s persistent, frustrating, and emotionally draining.
Patients often tell me:
“I exfoliate constantly and nothing changes.”
“My arms look spotty whatever I do.”
“I’ve had this since my teens, will it ever go?”
If that sounds familiar, you’re not alone. KP affects up to 40% of adults, and despite how common it is, it’s frequently misunderstood.
What Is Keratosis Pilaris?
Keratosis pilaris is a disorder of keratinisation, meaning the skin sheds keratin unevenly.
Instead of shedding smoothly:
Keratin builds up within hair follicles
This forms tiny plugs
Which appear as rough, raised bumps on the skin
These bumps may be:
Skin-coloured
Pink or red
Brown (more common in deeper skin tones)
The skin often feels like sandpaper or permanent goosebumps.
KP is not an infection, not acne, and not caused by poor hygiene.
Common Areas Affected by Keratosis Pilaris
KP most commonly appears on:
Upper arms
Thighs
Buttocks
Cheeks (especially in children and young adults)
Less commonly, it can affect:
Forearms
Lower legs
Jawline
Facial KP is increasingly common and is often mistaken for acne, rosacea, or folliculitis, leading to treatments that actually worsen it.
Why Does Keratosis Pilaris Happen?
KP is largely genetically determined. If you have it, there’s often a family history.
Contributing factors include:
Inherited skin-barrier differences
Dry or eczema-prone skin
Atopic conditions (eczema, asthma, hay fever)
Hormonal changes
Cold, dry weather (KP often worsens in winter)
Crucially, KP is not caused by dirt, blocked pores, or lack of exfoliation.
Why Exfoliation Alone Rarely Works
This is where many people struggle.
Because KP begins inside the hair follicle, aggressive exfoliation:
Irritates already-fragile skin
Increases redness and inflammation
Damages the skin barrier
Makes KP appear worse rather than better
Scrubs, loofahs, harsh acids, and over-exfoliation often exaggerate KP, particularly in sensitive or eczema-prone skin.
The Two Clinical Patterns of Keratosis Pilaris
KP usually presents as a combination of two patterns:
1. Textural (Non-Inflammatory) KP
Rough, bumpy texture
Minimal redness
Common on arms and thighs
2. Inflammatory KP
Red or pink bumps
Background redness
Often mistaken for acne
More common on arms and face
Understanding which pattern dominates helps guide treatment.
Can Keratosis Pilaris Be Cured?
The honest answer: no—but it can be significantly improved.
KP is a long-term skin tendency, not a disease to eliminate. Treatment aims to:
Smooth texture
Reduce redness
Improve comfort
Minimise flare-ups
Consistency matters far more than intensity.
What Actually Helps Keratosis Pilaris?
1. Skin Barrier First
KP skin is usually barrier-impaired.
This means:
Gentle, non-foaming cleansers
Avoiding stripping products
Prioritising moisturisation over exfoliation
Without a healthy barrier, active treatments often fail.
2. Smart Keratolytics (Not Over-Exfoliation)
Ingredients that help normalise keratin shedding include:
Urea
Lactic acid
Low-strength salicylic acid
Polyhydroxy acids (PHAs)
Best practice:
Introduce slowly
Use a few times per week
Always pair with rich moisturisers
More is not better with KP.
3. Anti-Inflammatory Support
For red or inflamed KP:
Calming ingredients matter more than acids
Niacinamide, azelaic acid, ceramides can help
Heat, friction, and tight clothing often worsen symptoms
Inflammation control is key to improving appearance.
Why KP Often Improves With Age (But Not Always)
Many people notice KP:
Softens in their 30s–40s
Becomes less inflamed over time
Improves with hormonal changes
Others find it persists, particularly on arms and thighs, making maintenance important.
The Emotional Impact of Keratosis Pilaris
KP is medically harmless, but emotionally significant.
Patients often:
Avoid sleeveless clothing
Feel self-conscious in summer
Worry their skin looks “unclean”
Feel frustrated after years of failed treatments
Dismissing KP as “just cosmetic” ignores its real impact on confidence.
Keratosis Pilaris and Sensitive Skin
KP commonly overlaps with:
Eczema-prone skin
Rosacea tendencies
Allergic conditions
This makes gentle, medical, individualised care essential. Trend-led or aggressive routines often backfire.
Managing KP in Real Life (Not Instagram Skin)
The realistic goal with KP is:
Softer skin
Less visible bumps
Reduced redness
Predictable flare control
Not poreless perfection.
When KP is well managed, it stops being the first thing you notice—and that’s a meaningful win.
Keratosis Pilaris Support in Hale, Cheshire
At our doctor-led clinic in Hale, we regularly see patients who’ve struggled with KP for years and have been told “nothing can be done.”
While KP isn’t something we cure, thoughtful guidance, barrier-focused skincare, and realistic expectations can make a genuine difference.
Frequently Asked Questions
Is keratosis pilaris acne?
No. KP is a keratinisation issue, not bacteria or blocked pores.
Is KP caused by diet?
There’s no strong evidence diet causes KP, though overall skin health influences inflammation.
Does KP worsen in winter?
Yes, cold weather and low humidity commonly worsen symptoms.
Can KP be scrubbed away?
No. Aggressive exfoliation usually makes it worse.
Is KP linked to eczema?
Yes. KP is more common in people with atopic (eczema-prone) skin.
References
DermNet NZ – Keratosis pilaris: https://dermnetnz.org/topics/keratosis-pilaris
NHS – Keratosis pilaris: https://www.nhs.uk/conditions/keratosis-pilaris/
British Association of Dermatologists PIL: https://www.bad.org.uk/pils/keratosis-pilaris
StatPearls (NCBI Bookshelf): https://www.ncbi.nlm.nih.gov/books/NBK546708/
Review article (PMC): https://pmc.ncbi.nlm.nih.gov/articles/PMC3681106/
Mayo Clinic – Diagnosis & treatment: https://www.mayoclinic.org/diseases-conditions/keratosis-pilaris/diagnosis-treatment/drc-20351152